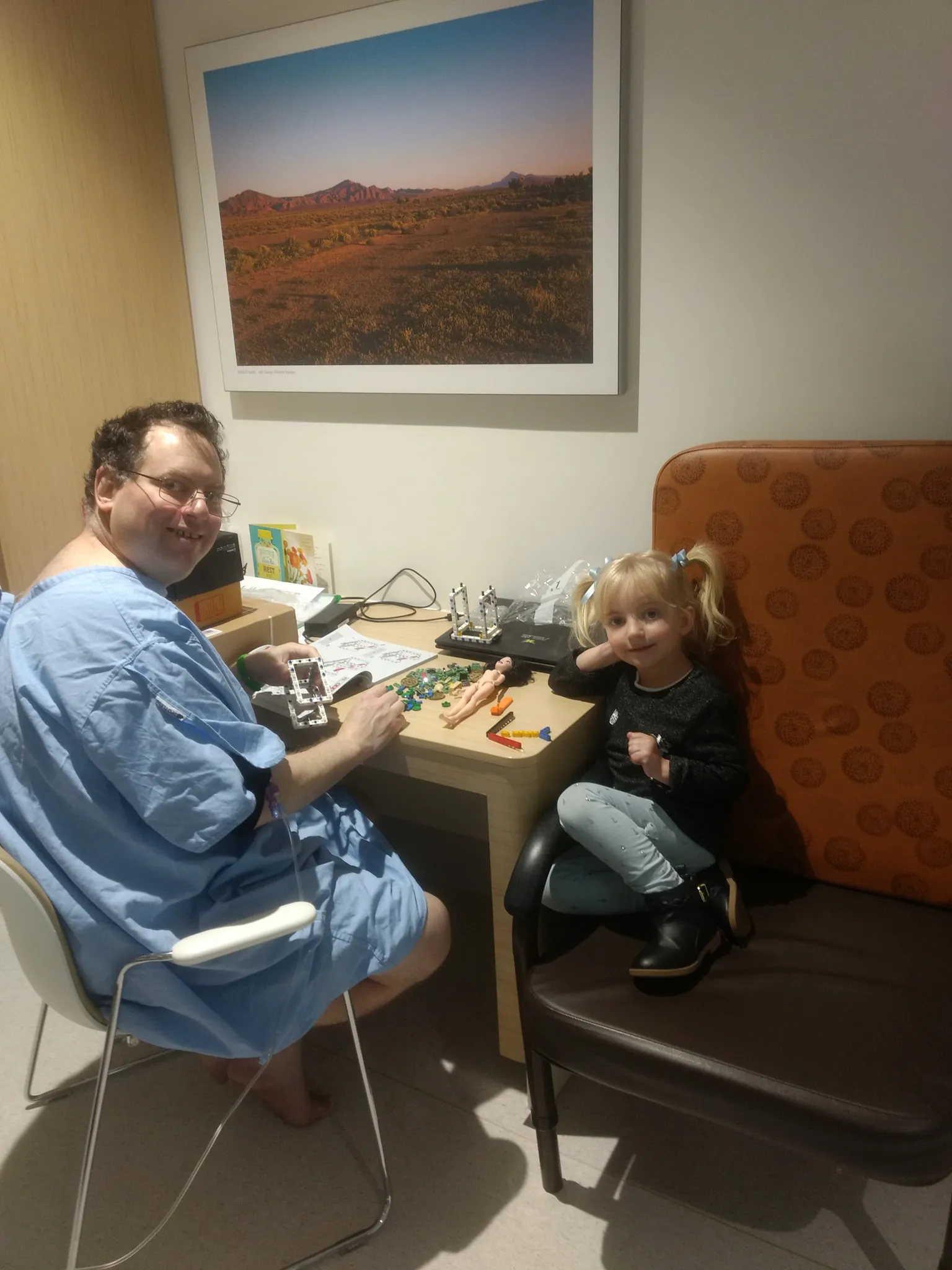
For Katrina Richards, a five-year delay in diagnosis was followed by a further wait for access to treatment.
Back in 2010, Katrina's illness started innocently enough – as a burning itch that she thought might
be caused by heat or an unknown irritant.
When the skin on her hands began to harden and split, she went to her doctor and embarked on a five-year quest for answers.
Tests
initially revealed an allergy to dust, and Katrina, 46, was prescribed
steroid
cream. When the soles of her feet started to crack and she noticed a
strange rash, she was sent to a dermatologist in Tamworth – two hours
from her family home in Narrabri.
Passed
between doctors who struggled to find a diagnosis, Katrina was
prescribed medication
that led to her losing her hair, as well as the skin on her neck and
chest. With symptoms worsening and still without answers, Katrina was
admitted to hospital to find her organs had started to shut down and
she'd put on 20kg of fluid in a week.
"I
had to give up work because my skin was in such bad shape," she
recalls. "I loved
my job and my co-workers, and it was really difficult to give that up. I
didn't want to leave the house because I felt I looked like a freak – I
became a hermit."
During this time of uncertainty, Katrina's relationship with her partner, Steven, was
also put under huge pressure, as it moved from an equal partnership to that of patient and carer.
"Our
relationship had been 50/50," says Katrina, "but suddenly Steven was
having to do
the cooking, cleaning, shopping and ironing, plus work and look after
kids. It was hard because I was used to working full-time, raising four
kids and still having a spotless home, and now I couldn't get out of
bed."
In
2012, Katrina was admitted to hospital for twice-daily wet bandaging to
try and manage
her condition – something that initially soothed her skin. However, the
task was then passed to community health, who – in her small country
town – only had the capacity to bandage her once a day. This meant
Steven had to do the bandaging at night – adding
yet more pressure to his workload.
Still
with no clear answers after five years of ill health, Katrina continued
to visit
specialists - undergoing numerous tests and prescribed a variety of
medications. She only got answers after a chance meeting with a
rheumatologist whose wife had been researching the early stages of the
type of blood cancer Katrina was eventually diagnosed
with: stage four, subcutaneous T-cell lymphoma.
"When
I was diagnosed I was scared," Katrina recalls, "because I thought, 'If
I'm at
stage four, what hope have I got to make it?' I was also angry and
frustrated – I didn't understand how a skin problem could be caused by
lymphoma, and I didn't know how pathology had missed it for so long."
With a clear diagnosis now in place, Katrina had to urgently relocate 530 km from the
family home to Sydney for treatment.
"It
was a huge change for the family, and for me," says Katrina. "For nine
months I just
wasn't home, and there was no guarantee of me ever coming home. Being
away from your family, you feel isolated - you're not part of your
family's life, even though you talk to them every day. You feel like
your life stops and everyone else's keeps going, because
you can't make plans - you don't know what's around the corner."
Katrina’s delay in diagnosis was followed by an agonising six-month wait for a drug she
needed but couldn't afford – one that was eventually made available to her on compassionate grounds.
"I
used to lie in bed at night and imagine I could feel my body just
multiplying these
horrible little cancer cells," recalls Katrina. "I'd think, 'This is
another day that I haven't had any treatment,' and I'd wonder, 'The
longer I wait, is this going to make my outcome less of a chance of a
good outcome?
As
part of her treatment, Katrina received a stem cells transplant –
something that was
made more difficult because she is of Indigenous descent, which can
make it even more challenging to find a match. Eventually, Katrina
achieved remission and was well enough to return to Narrabri. However,
the couple still had to make a weekly, 12-hour round
trip to hospital in Sydney – sometimes waiting four or five hours to
see a doctor before starting the long drive home.
Having
now been cancer-free for four years, Katrina feels gratitude for every
moment
with her family. If the national standards set out in the Leukaemia
Foundation’s new Set the Standard campaign had existed when Katrina
first attended her GP, Katrina may have been diagnosed sooner and had
access to the best possible cancer treatment – something
that drives her to advocate for the standards.
"It's
about time – it's so needed," she says. "If we had national standards,
it would
make a huge difference – because some people pass away without a
diagnosis. Blood cancer doesn't care what gender you identify as, what
race you are or how much money you have – it impacts all walks of life,
and everyone has the right to good healthcare."